excellent description of the process courtesy of USA Today
figures 1-3 : what a normal Vaccine trial looks like
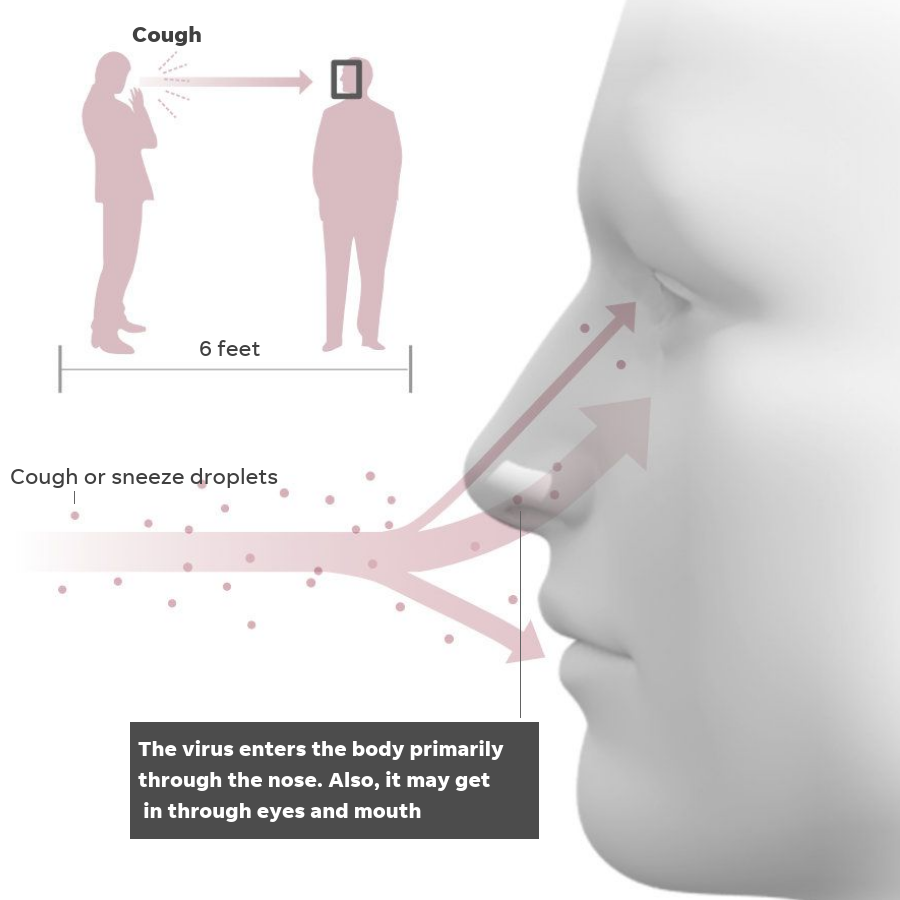
“It’s a respiratory virus and thus it enters through the respiratory tract, we think primarily through the nose,” according to a senior physician at Mass General. “But it might be able to get in through the eyes and mouth because that’s how other respiratory viruses behave.”
When the virus enters the body, it starts by attacking healthy epithelial cells of the respiratory tract and upper airway.
Fever, cough and other COVID-19 symptoms
It can take two to 14 days for a person to develop symptoms after initial exposure to the virus, Hirsch said. The average is about five days.
Inside the body, it begins infecting epithelial cells in the lining of the lung. A receptor protein of the virus then attaches to a host cell’s receptors this allows it to penetrate the cell. Inside the host cell, the virus begins to replicate until cell death. The virus starts in the upper respiratory tract; nose, mouth, larynx and bronchi.
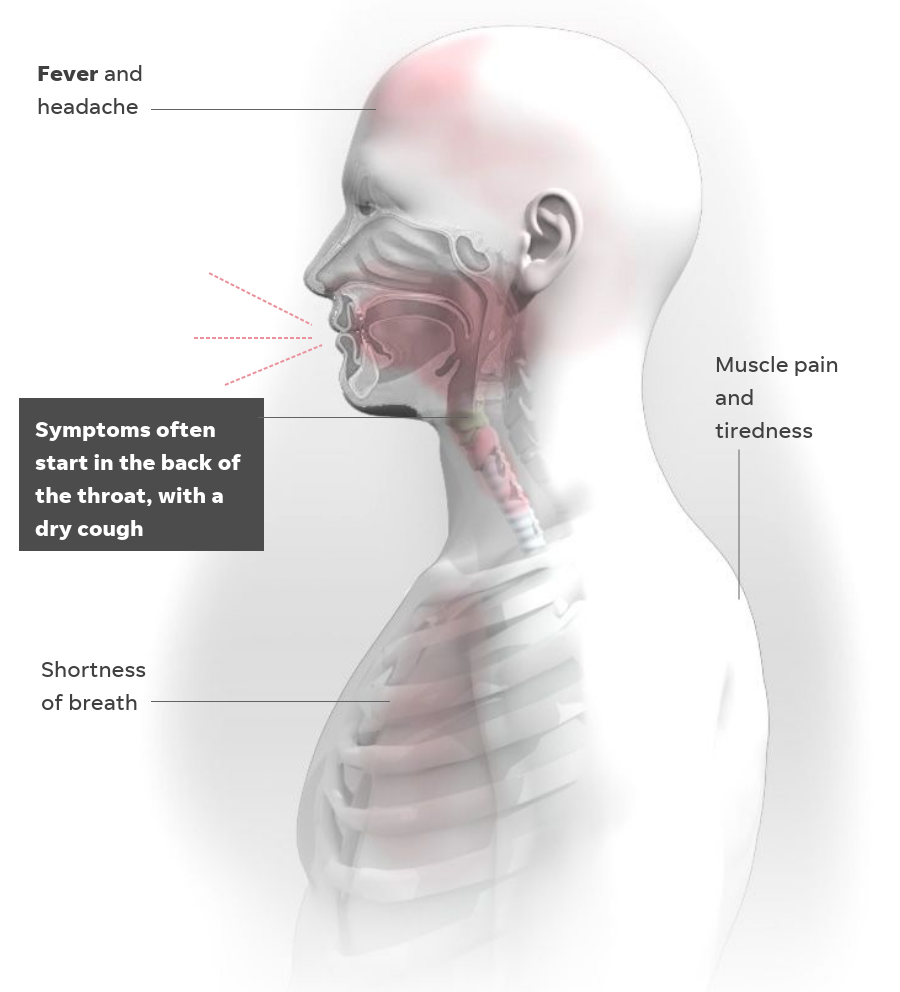
The patient begins to experience mild version of symptoms: dry cough, shortness of breath, fever and headache and muscle pain and tiredness, comparable to the flu.
Gastrointestinal symptoms nausea and diarrhea are also possible however this is rare.
Symptoms become more severe once the infection starts making its way to the lower respiratory tract.
Pneumonia and autoimmune disease
The WHO reported last month about 80% of patients have a mild to moderate disease from infection. A case of “mild” COVID-19 includes a fever and cough more severe than the seasonal flu but does not require hospitalization.
Those milder cases are because the body’s immune response is able to contain the virus in the upper respiratory tract, Hirsch says. Younger patients have a more vigorous immune response compared to older patients.
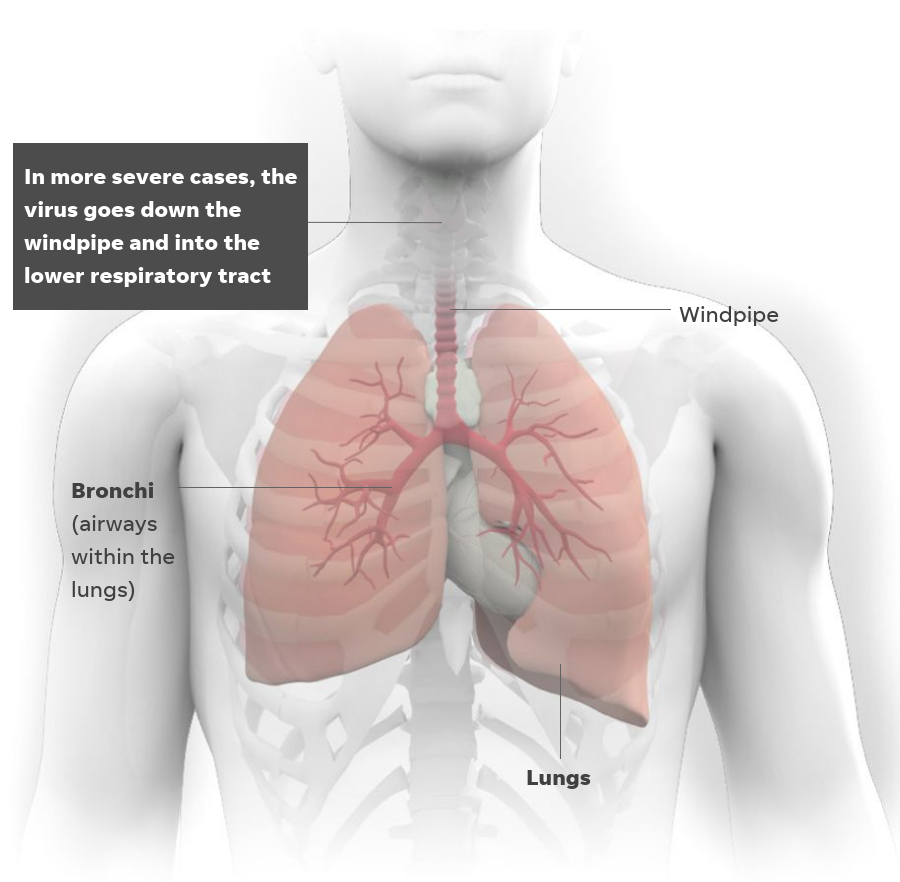
The 13.8% of severe cases and 6.1% critical cases are due to the virus trekking down the windpipe and entering the lower respiratory tract, where it grows more quickly
As the virus continues to replicate and journeys further down the windpipe and into the lung, it can cause more respiratory problems like bronchitis and pneumonia, according to Dr. Raphael Viscidi, infectious disease specialist at Johns Hopkins Medicine.
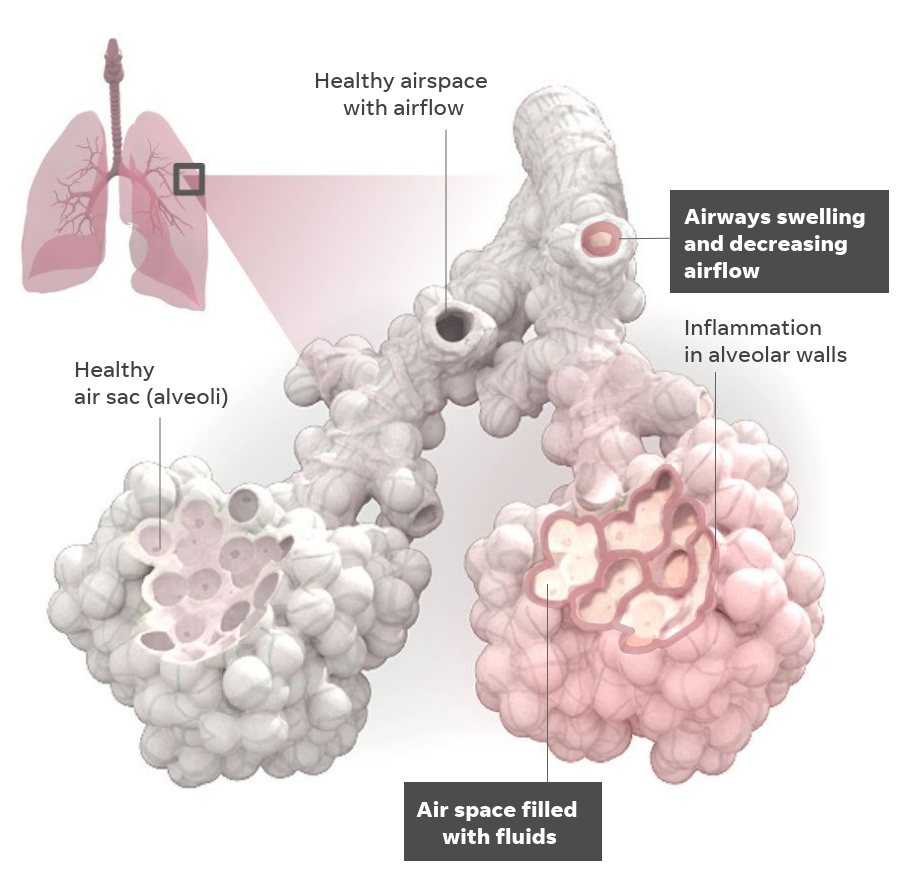
Pneumonia is characterized by shortness of breath combined with a cough and affects tiny air sacs in the lungs, called alveoli, Viscidi said. The alveoli are where oxygen and carbon dioxide are exchanged.
When pneumonia occurs, the thin layer of alveolar cells is damaged by the virus. The body reacts by sending immune cells to the lung to fight it off.
“And that results in the linings becoming thicker than normal,” he said. “As they thicken more and more, they essentially choke off the little air pocket, which is what you need to get the oxygen to your blood.”
So it’s basically a war between the host response and the virus,” Dr. Martin S. Hirsch, senior physician in the Infectious Diseases Services at. “Depending who wins this war we have either good outcomes where patients recover or bad outcomes where they don’t.”
Restricting oxygen to the bloodstream deprives other major organs of oxygen including the liver, kidney and brain.
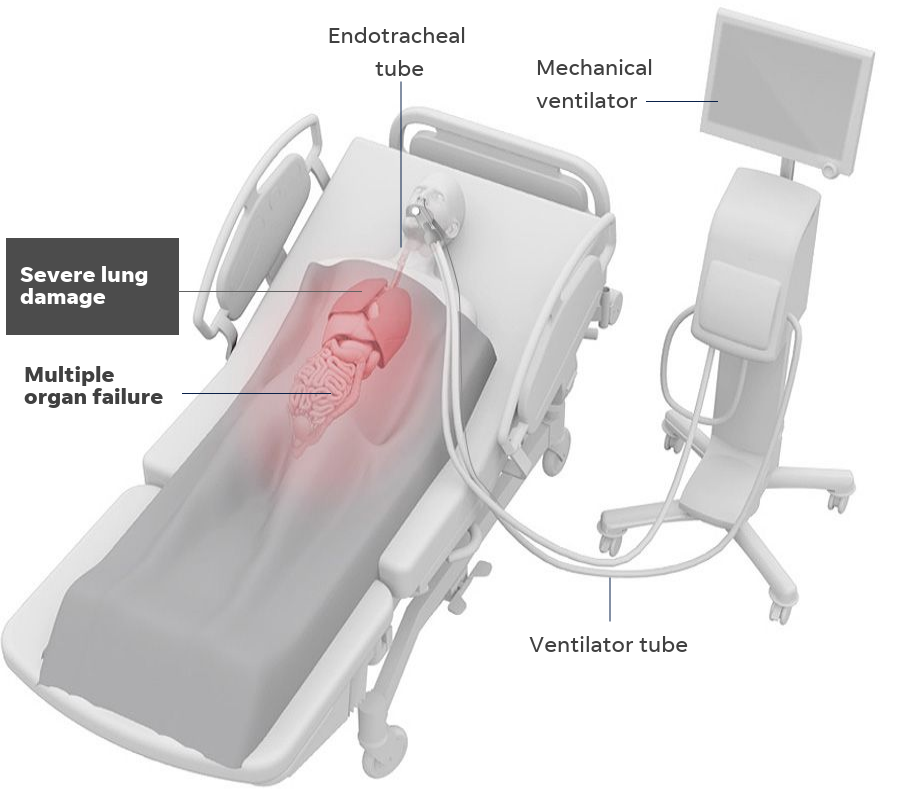
In a small number of severe cases that can develop into acute respiratory distress syndrome (ARDS), which requires a patient be placed on a ventilator to supply oxygen.
However, if too much of the lung is damaged and not enough oxygen is supplied to the rest of the body, respiratory failure could lead to organ failure and death.
Viscidi stresses that outcome is uncommon for the majority of patients infected with coronavirus. Those most at risk to severe developments are older than 70 and have weak immune responses. Others at risk include people with pulmonary abnormalities, chronic disease or compromised immune systems, such as cancer patients who have gone through chemotherapy treatment.
Viscidi urges to public to think of the coronavirus like the flu because it goes through the same process within the body. Many people contract the flu and recover with no complications.
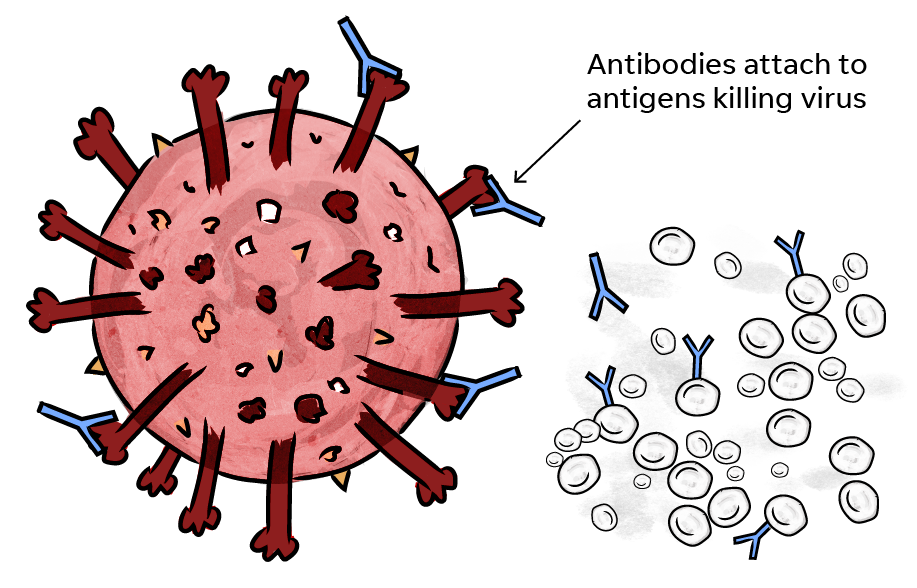
The good guys are your white blood cells, especially the ones called lymphocytes that produce antibodies.
These antibodies attach to antigens on the pathogens and prevent pathogens from invading other cells. Antibodies signal other white blood cells, which kill and remove the pathogens.
The problem is, a specific shape of antibody is needed. The human body has billions of white blood cells, each making its own special-shaped antibody. Only a few antibody shapes will be effective against the pathogen.
It can take several days for the immune system to produce enough properly shaped antibodies to kill the invading pathogens. During that time, a fast-acting pathogen, which can replicate billions of copies of itself, is a critical health threat.
Vaccines speed up the process by making the immune system believe it’s being attacked. After a vaccine primes your immune system, a number of white blood cells called memory cells are ready to make antibodies if the real pathogens attack.
“Even years later, you’re going to have these memory cells that will jump into gear,” Dr. Relman says.














































Recent Comments